STOPPING SPERM IN THEIR TRACKS
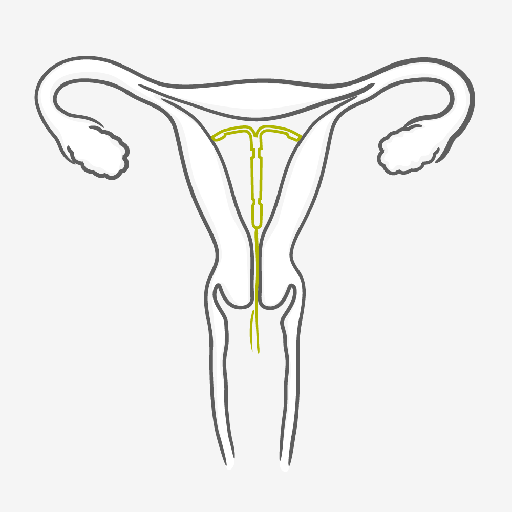
The IUS is a small, soft, T-shaped device with a reservoir containing the hormone progestogen that is placed in the womb by your healthcare provider. The IUS works by continuously releasing a low dose of progestogen from the intrauterine system into the womb. It thickens the mucus of your cervix, which makes it harder for sperm to move freely and reach the egg and it also thins the lining of your uterus. At 99.8% effectiveness, you’re about as protected as you possibly can be by a contraceptive method. It’s a great method for the super organized, the forgetful, the frequent traveller and pretty much anyone else who is keen on staying not pregnant. However, there are some individual risk factors that make an IUS not recommendable to some women. Therefore consult your healthcare provider in order to find out about your individual situation.

HOW TO
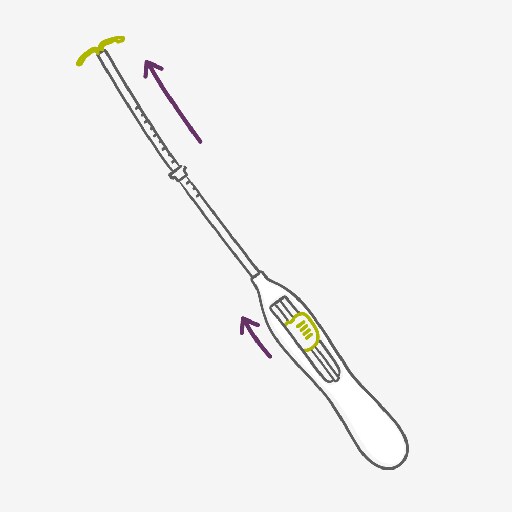
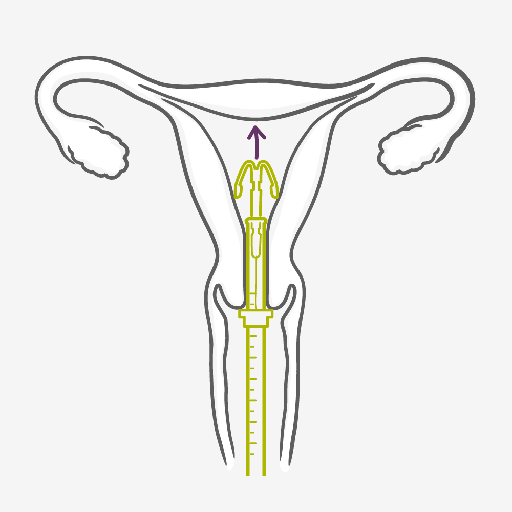
There really is nothing to using the IUS apart from a consultation with your healthcare provider to make sure whether it’s the right method for you. Once the IUS has been fitted by a well-trained healthcare provider, you’re highly protected from pregnancy for up to 5 years, depending on the type. After the IUS is taken out, the contraceptive effect wears off quickly and you can become pregnant as rapidly as women who have used no contraceptive at all.
PROS / CONS
- It can stay in place for up to 5 years (depending on the type), but can be removed any time.
- At 99.8%, it’s one of the most effective contraceptive methods
- It doesn’t interrupt sex
- Heavy periods can become lighter and less painful
- Some women may have shorter lighter or less frequent periods, which reduces the chances of becoming anemic
- Suitable for women who want long-acting reversible contraception for up to 5 years and wish to avoid daily, weekly or monthly regimens
- It can be used when breastfeeding
- Fertility returns to its previous level once the IUS is removed
- It requires a trained healthcare provider for insertion and removal
- Irregular bleeding and spotting can be common in the first 6 months of use
- Some women experience headaches, tenderness and acne after an IUS is fitted
- It may cause cramps and/or irregular bleeding
- Small risk of infection at insertion and of expulsion
- Does not protect against HIV infection (AIDS) and other sexually transmitted infections (STIs)
GIRLS TALK
FREQUENTLY ASKED QUESTIONS
An IUS insertion is usually well tolerated by most women. Some women may experience pain and dizziness after insertion, which usually settles after resting for a short time. Normal pain killers or local anesthesia may be applied to the uterine cervix prior to the insertion.
The IUS was not investigated for use as an emergency contraception.
The IUS must be inserted by a trained healthcare provider, who will follow the necessary procedure to ensure it is correctly positioned. Occasionally, the muscular contractions of the womb during menstruation may sometimes push it out of place or expel it. Very rarely it can perforate the wall of the uterus. If a user of an IUS experiences any unusual bleeding, pain or discomfort, the doctor or healthcare provider must be informed as soon as possible.
Neither you nor your partner should feel the IUS during sexual intercourse. If you do, sexual intercourse should be avoided until your doctor or healthcare provider has checked that the IUS is still in the correct position.

The IUD (Intrauterine Device) is a small plastic T-shaped device covered by copper or other metals which is inserted in the cavity of the womb. The IUS (Intrauterine System), is made of two components: the plastic T-shaped device and a cylinder containing progestogen hormone, which is released slowly from the system. The IUS and IUD have a number of different characteristics and work in a different way. Talk to your doctor or healthcare provider to find out which option is more appropriate for you.
Use of sanitary pads is recommended. If tampons are used, you should change them more frequently the first month after the IUS is inserted.
The progestogen released from the IUS causes the lining of the uterus to become very thin. Therefore it can change your menstrual periods so that you can have shorter or longer periods, lighter or heavier bleeding, or no bleeding at all. When the IUS is first inserted, before the lining becomes completely thinned out, women may have unpredictable spotting (a small amount of blood loss). This usually clears after the first months following insertion. If it does not clear, then you should see your doctor or healthcare provider to make sure there is not another cause for the bleeding.
Many women with an IUS will experience less and lighter bleeding after the IUS is fitted. Some women may not have any periods at all anymore.
An IUS can be left in place for up to three or five years depending in the type. After this time, it will need to be replaced with a new device. If this method of contraception has worked well for you, and if you still wish to use a long-term contraceptive option, then you can discuss with your healthcare provider about continuing with this method.