YOUR FAVOURITE INJECTION
The contraceptive injection is a shot that contains the hormone progestogen that stops your body from releasing eggs and thickens the mucus at the cervix. You need one shot either once every two months or once every three months from a healthcare provider. However once injected, it is not reversible, i.e. in case of side effects it cannot be stopped. The way it works is similar to the pill, or the ring, except you don’t have to remember to take it every day or week, but it probably isn’t the best choice for those scared of needles.

HOW TO
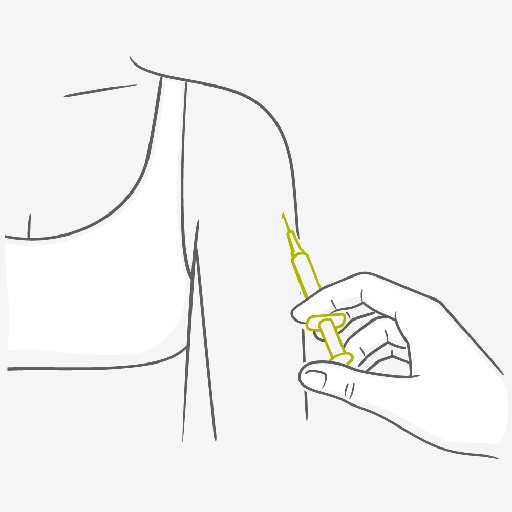
Firstly you’re going to need to talk to your healthcare provider. As with most contraceptives, they aren’t the ideal choice for everyone so getting advice from a professional is something we always recommend. If you decide the contraceptive injection is a method you’re interested in your healthcare provider will do it for you. Then, depending on the type of shot you get, you’ll just need to go back every two months or every three months for another top up and you’ll be highly protected in between.
PROS / CONS
- It lasts for 2 or 3 months
- It permits sexual spontaneity and doesn’t interrupt sex
- It doesn`t require daily or weekly attention
- It can offer an alternative to those affected by the hormone estrogen
- It can be used when breastfeeding
- It may reduce heavy and painful periods for some women
- It requires keeping track of the number of month used
- It may cause some people to suffer headaches and mood swings
- It may cause headache, weight gain, abdominal discomfort
- It may take up to one year for your period and fertility to return after stopping injection
- It may cause disrupted periods
- You may lose bone density if you get the shot for more than 2 years in a row
- Does not protect against HIV infection (AIDS) and other sexually transmitted infections (STIs)
GIRLS TALK
FREQUENTLY ASKED QUESTIONS
The injection must be given by a healthcare provider. Depending on where you live, you can have the injection done at your local doctors or family planning clinic.
You do need to have the injection once every two or three months, depending on the type of injection you have. The amount of hormone which is injected to prevent unintended pregnancy will only last around 8-12 weeks depending on the type, so if you miss an injection you will not be protected against pregnancy.
If you are sexually active and do not currently wish to have children, you can continue having the injections to protect against pregnancy, providing you find the method suits you and you have regular check-ups with your doctor or healthcare provider.
No. There may be a delay in regaining fertility after stopping monthly injections, but in time the woman will be able to become pregnant as before, although fertility decreases as women get older. The bleeding pattern a woman had before she used injectable contraceptives generally returns a few months after the last injection. Some women may have to wait a few months before their usual bleeding pattern returns.
Periods and fertility may take up to a year to return after stopping injections, depending on the type of injectable, and this may vary from woman to woman.
Some women do experience weight gain, if this happens to you, speak with your healthcare provider, it may be that an alternative form of hormonal contraception is better suited to you.
Some women think that the next injection should only be given when the next bleeding begins. Bleeding episodes should not guide the injection schedule. However, a woman should receive the injection every 8 weeks or every 12 weeks depending on the type. The timing of injections should not be based on her monthly bleeding.
Generally, no. Some women using injectables report these complaints. The great majority of injectables users do not report any such changes, however, and some report that both mood and sex drive improve. It is difficult to tell whether such changes are due to injections or to other reasons. There is no evidence that injectable contraceptives affect women’s sexual behavior.
When you use injectable contraceptives you may have bleeding and spotting between periods. The menstrual bleeding may vary from slight staining between menstrual periods to breakthrough bleeding, which is a flow much like a regular period. It occurs most often during the first few months of usage, but may also occur after you have been using the contraceptive injection for some time. Such bleeding may be temporary and usually does not indicate any serious problems. It is important to continue using the injections on schedule. If the irregular bleeding or spotting is heavy or lasts for more than a few days, you should consult your doctor or healthcare provider.